The Gut Barrier: The Missing Link Between Your Gut and Hormones
The Truth I Had to Accept as a Nutritionist
When I started my journey as a nutritionist, I genuinely believed I was helping my patients fix their health at the root. I focused on clean eating, balanced meals, calorie control, and the right supplements for hormones. And to be fair, many of my patients did see results initially—weight improved, cycles became more regular, and lab reports looked better.
But over time, I started noticing a pattern that I couldn’t ignore. The same patients would come back.
PCOS that never fully resolved, Thyroid that stayed sluggish, Bloating that kept returning, Fatigue that didn’t match their “healthy lifestyle.”
And the most frustrating part? They were doing everything right.
That’s when I realized something uncomfortable but important: I was not truly addressing the root cause. I was managing symptoms.
I was looking at hormones, diet, and reports in isolation—without asking the deeper question
Why is the body behaving this way in the first place?
That question led me into functional medicine and the microbiome. And that’s where things started making sense.
Because most of these conditions didn’t begin with hormones.
They began much deeper.
They began at the level of the gut barrier.
What is the Gut Barrier (And Why It’s Not What You Think)
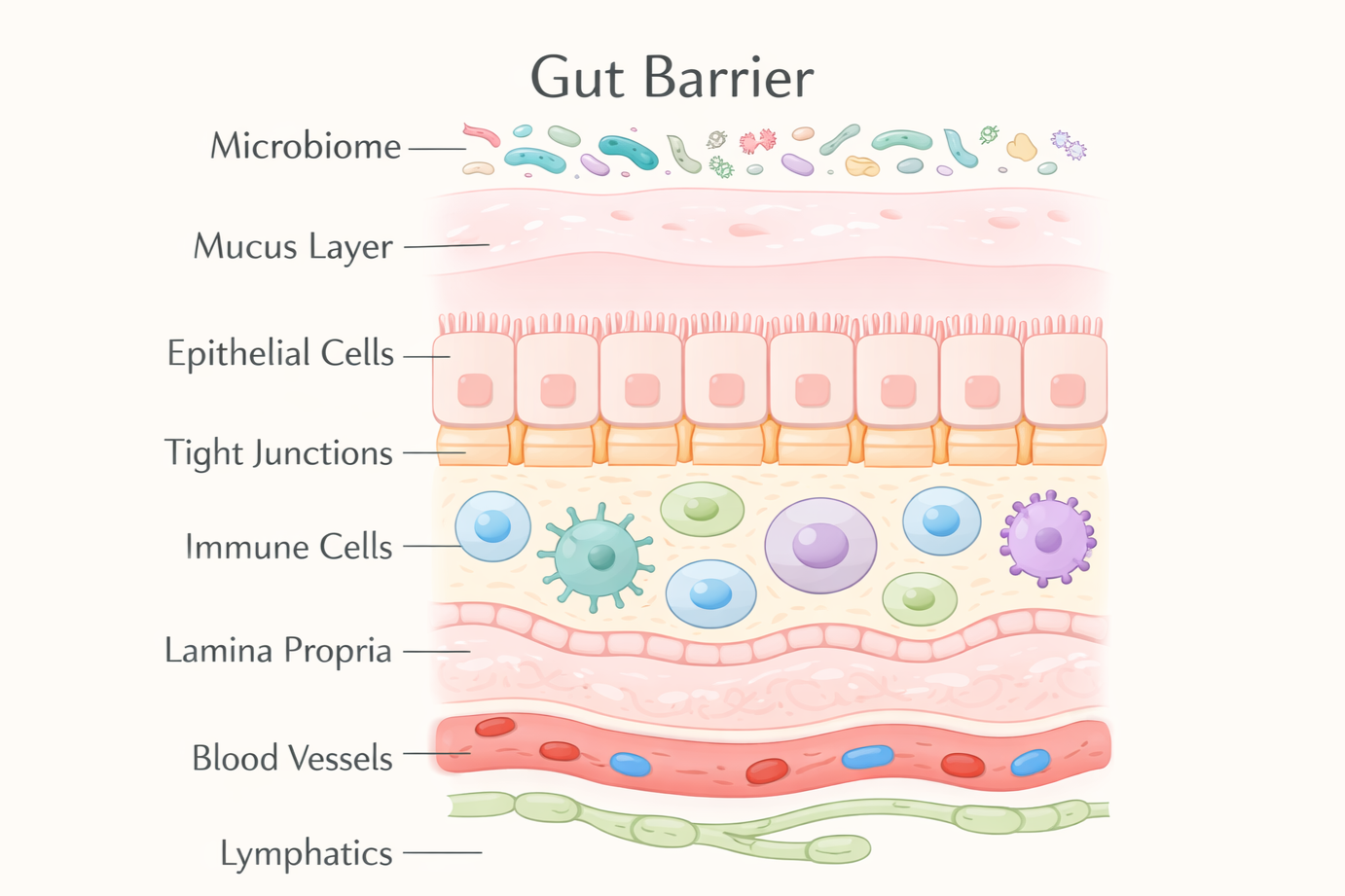
Healthy Gut Barrier
Most people think of the gut as just a digestive organ.
It’s not.
Your gut is actually a highly intelligent barrier system that decides what enters your body and what stays out.
It consists of four key layers:
The microbiome (good and bad bacteria)
The mucus layer
The intestinal lining (epithelial cells with tight junctions)
The immune system (GALT)
These layers are in constant communication with each other, making the gut barrier a dynamic, selectively permeable system—not a static wall.
Its job is simple but critical:
Let nutrients in
Keep toxins, bacteria, and inflammatory compounds out
When this system works well, your body stays in balance.
When it doesn’t, everything starts to shift.
Watch a complete Webinar on: Microbiome for Gut & Hormonal health
How the Gut Barrier Breaks Down
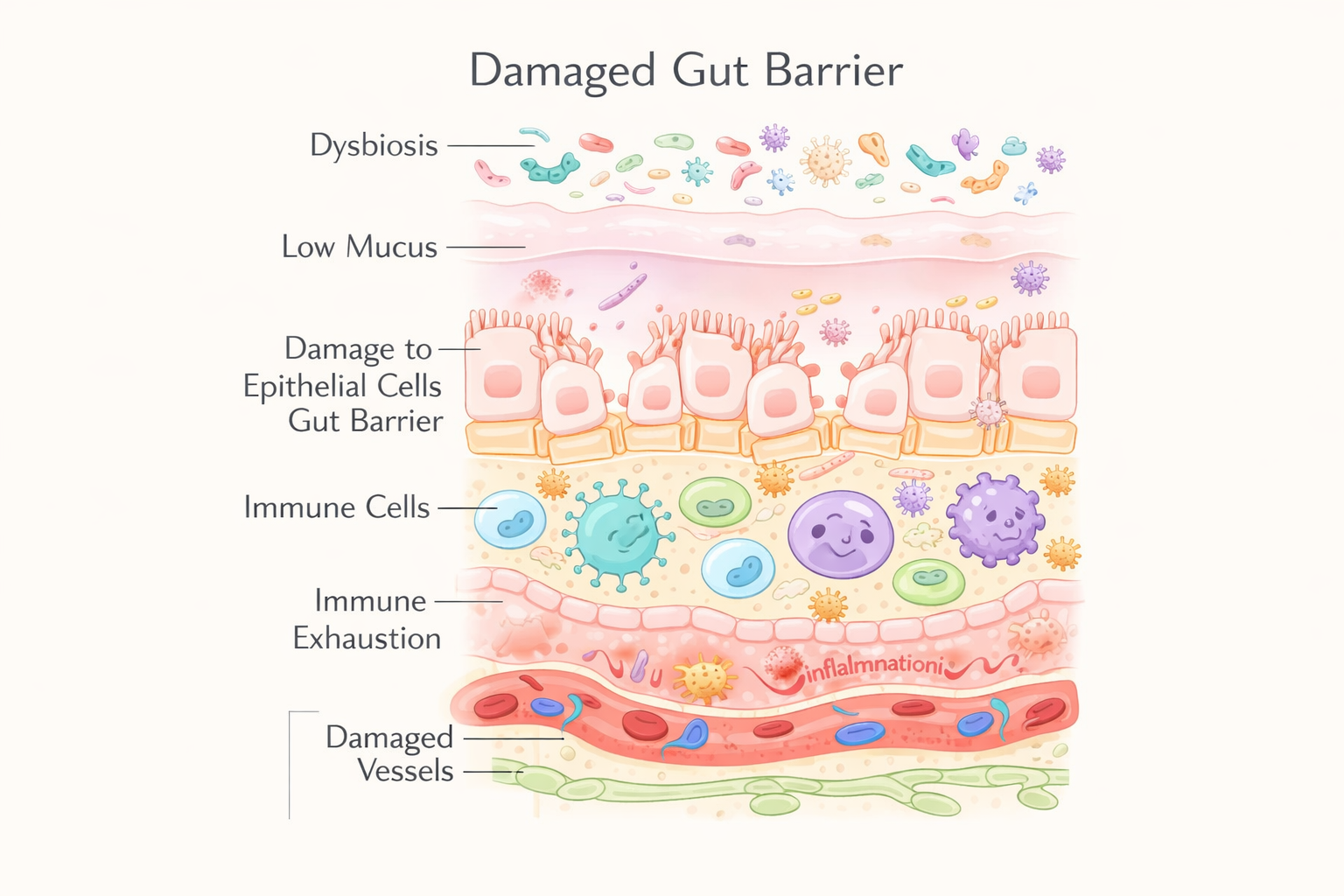
Damaged Gut Barrier
Gut issues don’t start as “leaky gut” overnight. It’s a gradual, layered breakdown. It typically follows this sequence:
1. Early dysfunction
Microbial imbalance (dysbiosis)
Reduced immune tolerance
Lower secretory IgA
2. Structural compromise
Mucus layer thinning
Poor epithelial repair
Weakening of tight junctions
3. Advanced breakdown
Increased intestinal permeability
Toxins crossing into bloodstream
Systemic inflammation
This progression—from a healthy barrier to endotoxemia—is clearly described in clinical models of gut barrier dysfunction.
The Real Problem: Endotoxemia
Once the barrier is compromised, a major shift happens. Fragments of bacteria—especially lipopolysaccharides (LPS)—start leaking into circulation. This is called metabolic endotoxemia.
LPS is not just another toxin. It is highly inflammatory and triggers a strong immune response by activating receptors like TLR4 and CD14.
This creates a state of chronic, low-grade inflammation—the kind that doesn’t always show up clearly on reports but slowly disrupts the entire body. And here’s what most people don’t realize: You can have endotoxemia without any gut symptoms.
I explained this in detail in my Webinar, you can watch it now- Microbiome for Gut & Hormonal Health
Why This Directly Affects Your Hormones
This is where everything connects.
When endotoxemia and inflammation are present, your body shifts into a survival state. Hormones are no longer a priority.
1. Cortisol and Stress Response
Inflammation activates the stress response, increasing cortisol levels and disrupting the nervous system.
At the same time, chronic stress itself worsens gut barrier function by reducing secretory IgA and weakening mucosal defenses.
This creates a vicious cycle: Stress → Gut damage → More inflammation → More stress
2. Sex Hormones (PCOS, Estrogen, Testosterone)
Endotoxemia has been directly linked to:
Suppressed sex hormone production
Poor ovarian function
Increased androgen levels
Which is why conditions like PCOS and hormonal imbalances are often connected to gut dysfunction.
3. Insulin Resistance
LPS drives:
Adipose inflammation
Impaired leptin signaling
Reduced insulin sensitivity
This becomes the foundation for:
PCOS
Belly fat
Sugar cravings
Metabolic dysfunction
4. Thyroid Function
Chronic inflammation from endotoxemia:
Impairs thyroid signaling
Affects T4 to T3 conversion
Increases autoimmune risk
This is why many thyroid cases don’t improve with just medication or nutrition alone.
Why Your Symptoms Don’t Always Look “Digestive”
One of the biggest misconceptions I see:
“If I don’t have gut issues, my gut must be fine.”
But gut barrier dysfunction often shows up as:
Fatigue
Brain fog
Acne or skin issues
Mood swings
Joint pain
Sugar cravings
These are commonly reported patterns associated with barrier dysfunction. Because LPS doesn’t just affect the gut—it affects the entire system.
If you want to learn more about these symptoms then you can join my Free Telegram Community, where you can get the access of regular webinar to educate yourself on Functional Approach for treating your Gut and Hormonal Symptoms.
The Role of Diet (And Why “Healthy Eating” Isn’t Always Enough)
Even diet plays a more nuanced role than we think.
For example:
High saturated fat intake can increase LPS absorption and worsen endotoxemia
Low fiber intake reduces beneficial bacteria and short-chain fatty acids (like butyrate) needed for repair
A high-fat, low-fiber meal has been shown to increase endotoxin levels post-meal
On the other hand:
Omega-3 fats help reduce endotoxemia
Fiber supports gut repair and microbial balance
Polyphenols improve barrier function
This is why simply “eating clean” without understanding your gut environment often isn’t enough.
Homemade Bone Broth can really be a soft start to your gut healing. Have a look at the recipe. In fact, minerals are also extremely important for gut repair, you can incorporate that too in your diet.
The Real Root Cause Framework
Instead of looking at health like this:
Hormones → Symptoms
You need to start seeing it like this:
Gut Barrier → Inflammation → Hormonal Disruption → Symptoms
Because in most chronic cases, the gut barrier is not a side issue.
It is the starting point.
Research now recognizes gut barrier dysfunction and endotoxemia as upstream drivers of chronic disease, often appearing long before visible symptoms.
My final thought:
At this stage in my practice, I don’t look at hormones as the starting point anymore.
I look at the gut barrier.
Because what I’ve consistently seen is this—when the gut barrier is compromised, the body is constantly in a low-grade inflammatory state. And in that state, no amount of diet correction or supplementation can create lasting hormonal balance.
This is also why quick fixes don’t work long-term. You might see temporary improvement, but unless the underlying dysfunction is addressed, the system eventually falls back into the same pattern.
That shift in perspective has completely changed the way I approach cases now. And more importantly, it has changed the kind of results my patients are able to achieve.
References:
Belkaid Y, Hand TW (2014) – Role of the microbiota in immunity and inflammation (Science) – https://doi.org/10.1126/science.1243489
Brandtzaeg P (2013) – The mucosal immune system and its integration with the mammary glands (Nature Reviews Immunology) – https://doi.org/10.1038/nri3468
Macia L et al. (2012) – Microbial influences on epithelial integrity and immune function (Immunological Reviews) – https://doi.org/10.1111/j.1600-065X.2011.01080.x
Kelly CJ et al. (2015) – Microbiota-derived SCFAs and intestinal barrier function (Nature Reviews Gastroenterology & Hepatology) – https://doi.org/10.1038/nrgastro.2015.186
de Punder K, Pruimboom L (2015) – Stress induces endotoxemia and inflammation (Frontiers in Immunology) – https://doi.org/10.3389/fimmu.2015.00223
Furusawa Y et al. (2013) – Butyrate induces regulatory T cells (Nature) – https://doi.org/10.1038/nature12721
Cani PD et al. (2008) – Gut microbiota and metabolic endotoxemia (Diabetes) – https://doi.org/10.2337/db07-1403
Johansson MEV et al. (2011) – Mucus layers and barrier protection (Cell Host & Microbe) – https://doi.org/10.1016/j.chom.2011.05.015